
Collagen in women and its unique functions
What is collagen? Collagen in women, men and nearly all animals is a fibrous/fibrillar protein that constitutes the connecting tissues of the human body. What do we mean by this? This includes our:...

Hidden Stress Triggers?
Hidden Stress Triggers? If I’m stressed by these triggers, are they actually hidden? Stress triggers are not always obvious, sometimes they can be completely subconscious and autonomously taken car...
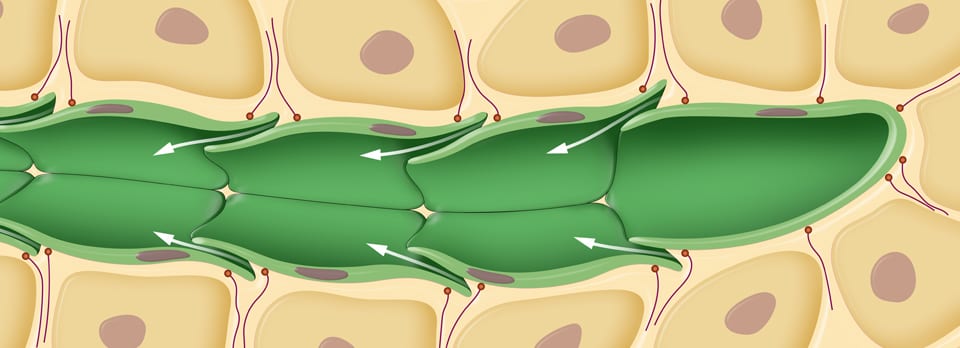
Lymphatic Health - Looking after your Lymph
‘Lymphatic system’ is a term I’m sure we are all familiar with now with the blessing of media health trends and the internet, but do we really know to the full extent the lymphatic system’s functio...
Gut Microbiome | A Guide To What It Is
Oestrogen–Gut Microbiome Axis: Physiological and Clinical Implications Within each human gastrointestinal tract there is an exclusive combination of different communities of organisms, including ba...










